The National Bureau of Disease Control and Prevention said that the epidemic situation in COVID-19 may rebound around the Spring Festival, and the harm of new strains will be explained in detail.
Lian Junxiang and Xu Hanyi recently held a press conference in the State Council Press Office. The relevant person in charge of the National Bureau of Disease Control and Prevention said that due to the sharp increase in personnel flow during Spring Festival travel rush, it is expected that the epidemic situation in COVID-19 may rebound to some extent before and after the Spring Festival, and many respiratory diseases will continue to appear alternately or jointly in many parts of the country.
So, what is the toxicity of the new strain JN.1 in COVID-19? Will influenza and COVID-19 cross-infect?
one
The number of people infected with JN.1 strain in China is increasing.
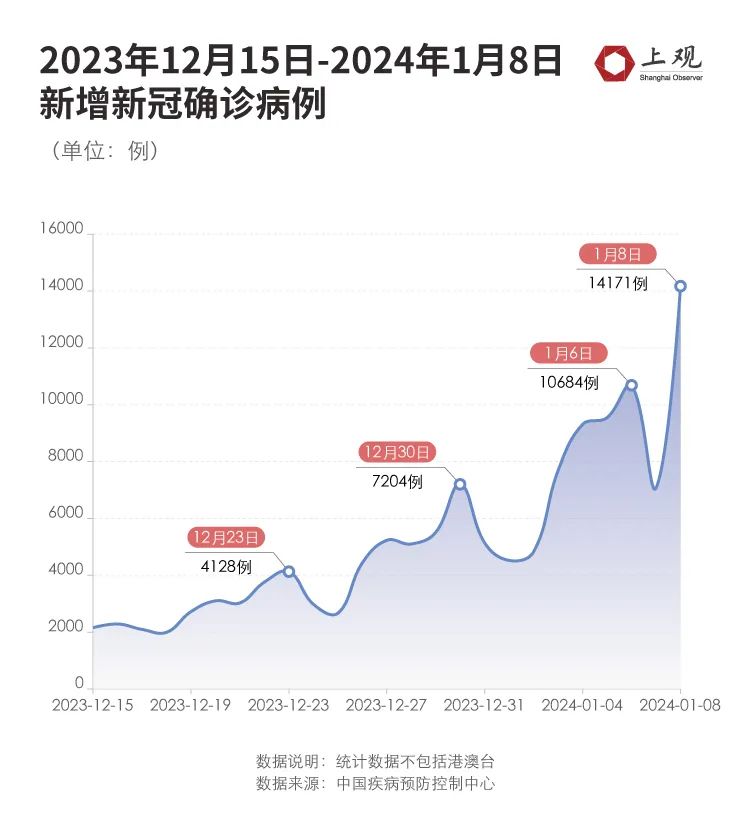
According to the data of China Center for Disease Control and Prevention, the number of cases in COVID-19 increased from the end of last year to the beginning of this year.
On January 6th, this year, the number of newly confirmed cases exceeded 10,000 for the first time, reaching 10,684. The number of positive detections in the last week has increased significantly.
At present, the mainstream strain is still EG.5 and its subfamilies, but the number of people infected with the latest JN.1 strain is increasing. As Spring Festival travel rush is coming, the epidemic of the virus may still be variable.
2
The mortality of new strains in COVID-19 is not high.
So, how harmful is the latest JN.1?
According to the global data, the spread of Covid-19 JN.1 is rapid, but the risk has not improved.
JN.1 is a second-generation subfamily of Omicron BA.2.86 mutant, which was first detected in Luxemburg at the end of August last year.
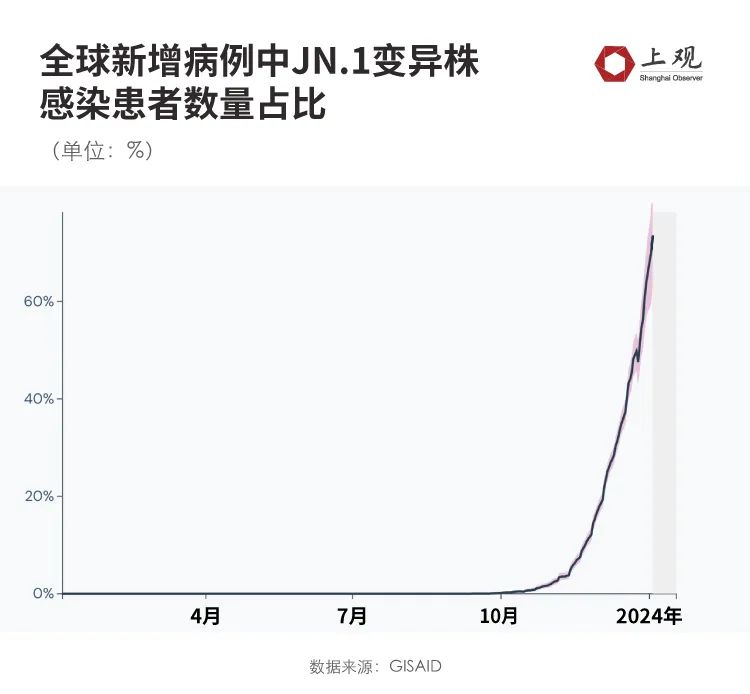
According to the latest data from GISAID, JN.1 began to spread around the world in November last year, and it took only one month to become the global mainstream strain, accounting for 50% of the new cases every day. At present, this proportion has exceeded 70% and spread to at least 59 countries and regions around the world.
The rapid transmission is also reflected in the level of virus activity in wastewater. The higher the value of this indicator, the wider the spread of the virus.
According to the data of the US Centers for Disease Control and Prevention (hereinafter referred to as CDC), the concentration level of Covid-19 in wastewater in the United States was 12.85 in the week of December 30th, reaching the second highest level in history since the outbreak of COVID-19 epidemic in the United States.
According to relevant scholars, compared with the previous Covid-19, JN.1 virus has acquired a key new mutation, so its spreading ability is stronger.
Judging from the hospitalization and mortality, the influence of JN.1 did not exceed that of the previous strain.
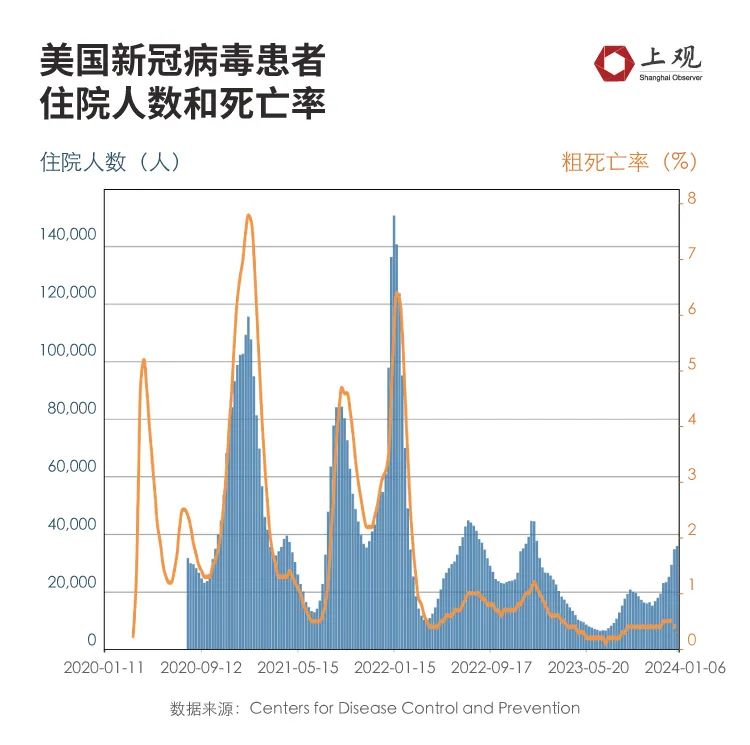
According to the data of CDC in the United States, in the week of January 6th, there were 35,800 new hospitalized applicants in COVID-19, with an average of about 11 per 100,000 people.
Although the trend has increased, it is not too serious compared with the previous peak. At the beginning of 2022, the number of people applying for hospitalization in the United States due to Covid-19 infection peaked at about 45.5 per 100,000 people, which is 4.4 times of the current level.
Judging from the death situation, the number of people who died of COVID-19 infection in the United States is decreasing.
In the week of January 6th, the number of people who died of Covid-19 infection was 0.3 per 100,000 people. Last year’s peak was 1.2/ 100,000 people, which is also about four times the current level.
If compared with 2020, the gap is bigger, about 26 times as much as the current one.
three
It is unlikely that influenza will merge with COVID-19.
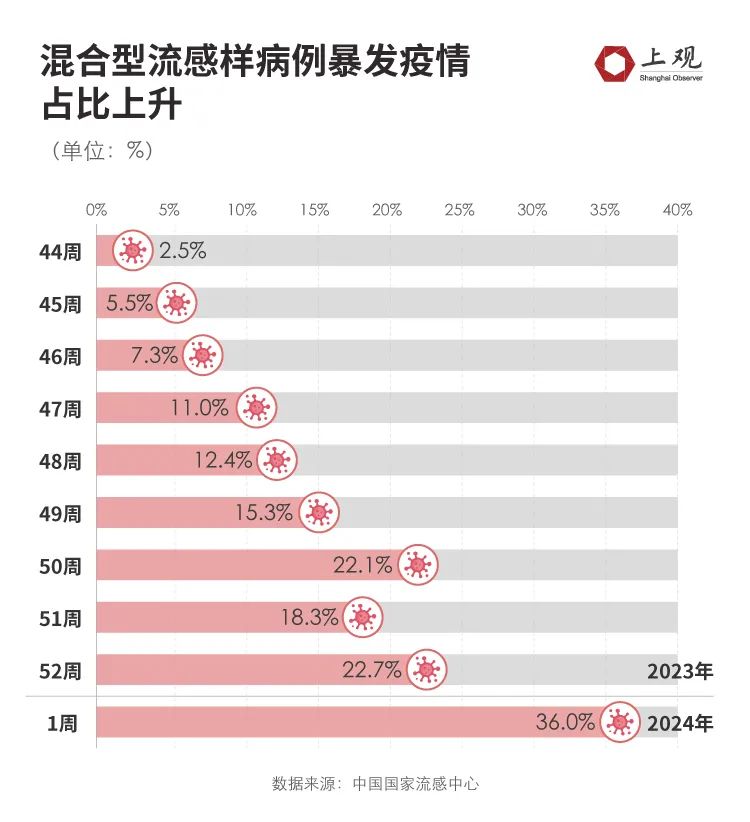
At present, the positive rate of influenza virus detection in China has declined, but among them, the proportion of B-stream is increasing, and the proportion of mixed infection is increasing recently. It may be infected at the same time, or it may be that "A stream is just right and B stream is recruited".
According to the data of China National Influenza Center, in the first week of 2024, the proportion of mixed infection increased to 36%, compared with only 12.4% a month ago.
With the spread of JN.1, will people who have had the flu still be infected with COVID-19?
Judging from the research data, it is possible, but the proportion is not high.
According to a paper published two years ago by scholars from the University of Aix-Marseille, 54 related studies around the world were collected and analyzed, including the data of about 18,000 patients infected with COVID-19.
The results showed that only 0.7% of the patients were co-infected with COVID-19 and influenza, that is to say, only about 140 of the 18,000 patients were co-infected with Covid-19 and influenza virus.
But compared with B-stream, A-stream is more likely to be infected with COVID-19.
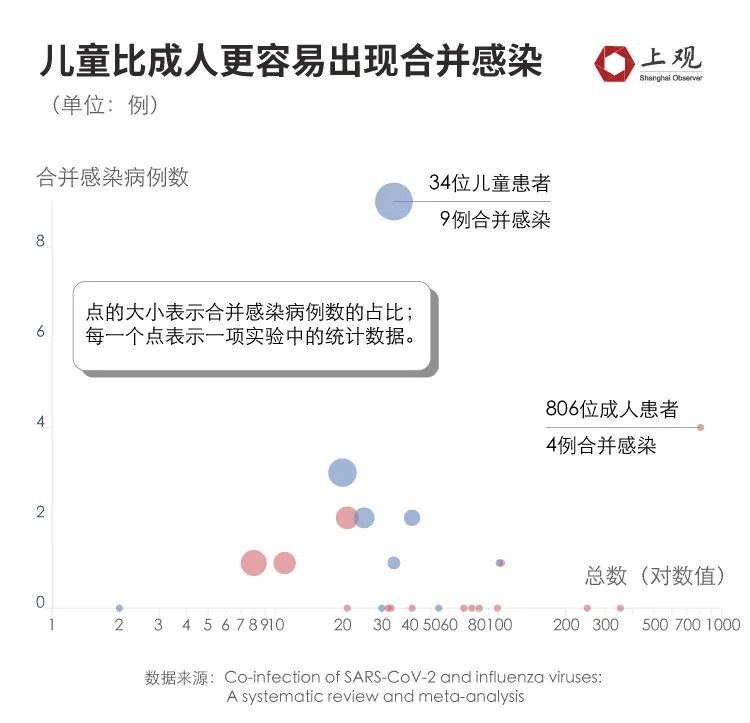
The data showed that among 143 patients with concurrent infection, 74% were infected with influenza A, 20% were infected with influenza B, and only one patient was infected with three viruses at the same time, with a low probability. Refined to the age of patients, children are more likely to be infected than adults.
The data shows that the proportion of children with infection is 3.2%, which is about 10 times as much as that of adult patients (0.3%).
four
Complicated with infection or aggravated illness
Although the possibility of concurrent infection is very low, once infected, it may aggravate the condition.
As early as 2021, the national key experiment of virology found that in the experimental mice, co-infection would cause more cells and tissues in the body to be attacked by the virus, which would lead to more serious lung pathological reactions, a large number of cell infiltration and obvious alveolar necrosis [2].
From the comparison of patients’ data, co-infection does lead to more serious symptoms of patients.
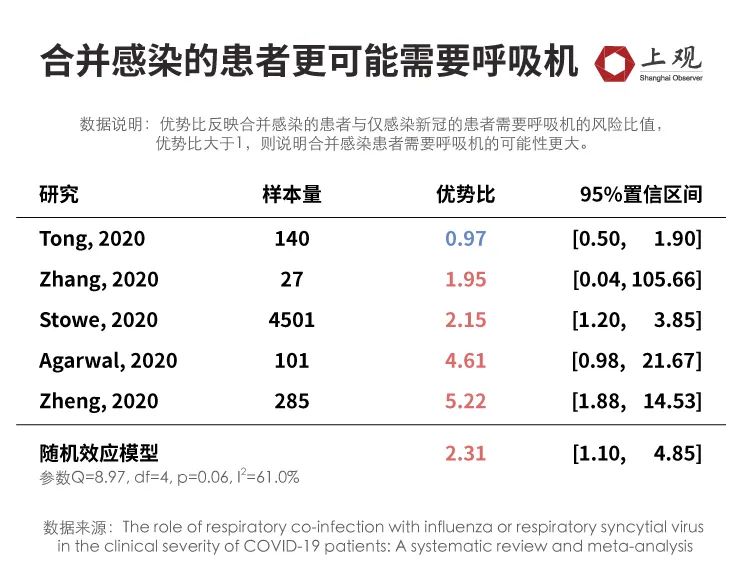
According to the paper published by Nanjing Medical University in 2022 [3], compared with patients infected with COVID-19 alone, patients with combined infection are more likely to need a ventilator, and the risk is 2.31 times that of patients infected with alone.
Among them, the risk of using a ventilator with COVID-19 and H1N1 infection is higher, which is 5.04 times that of single infection.
Symptoms mainly focus on respiratory complications, such as acute hypoxic respiratory failure, acute respiratory distress syndrome, heart injury and acute kidney injury.
Not only that, patients with infection are also more likely to live in ICU.
Research shows that [3], the risk of patients with co-infection staying in ICU is 2.09 times that of patients with single infection.
According to the paper published in the International Journal of Epidemiology in 2021 [4], in the face of co-infection, the elderly population is more likely to be seriously ill and more likely to cause life-threatening.
For example, among patients aged 50-59, 60% were admitted to ICU after infection, while the proportion of single infection was 24%. In patients aged 80 and above, the proportion of death after infection was 66.7%, which was also higher than that of single infection (46.5%).
However, co-infection may not increase the risk of death. Studies have shown that [3], there is no significant correlation between co-infection status and death.
Including the elderly, children and high-risk groups with basic diseases, it is necessary to pay attention to timely differential diagnosis and take related drugs after symptoms of upper respiratory tract infection, so as to alleviate symptoms, shorten the course of disease and reduce the risk of severe illness and hospitalization.
Paper citation:
【1】Dao, T. L., Colson, P., Million, M., & Gautret, P. (2021). Co-infection of SARS-CoV-2 and influenza viruses: a systematic review and meta-analysis. Journal of Clinical Virology Plus, 1(3), 100036.
【2】Bai, L., Zhao, Y., Dong, J., Liang, S., Guo, M., Liu, X., … & Xu, K. (2021). Coinfection with influenza A virus enhances SARS-CoV-2 infectivity. Cell research, 31(4), 395-403.
【3】Cong, B., Deng, S., Wang, X., & Li, Y. (2022). The role of respiratory co-infection with influenza or respiratory syncytial virus in the clinical severity of COVID-19 patients: A systema tic review and meta-analysis. Journal of Global Health, 12.
【4】Stowe, J., Tessier, E., Zhao, H., Guy, R., Muller-Pebody, B., Zambon, M., … & Lopez Bernal, J. (2021). Interactions between SARS-CoV-2 and influenza, and the impact of coinfection on disease severity: a test-negative design. International Journal of Epidemiology, 50(4), 1124-1133.
Original title: "The National Disease Control Bureau said that the epidemic situation in COVID-19 may rebound around the Spring Festival, and the harm of new strains is detailed."
Read the original text